|
5 One identified problem with the current healthcare system is that the three aims seem to be addressed independent of one another. 9 All of the components of the Triple Aim need to be considered when improving care because improving one may bring about undesired results in another. In December, Berwick described the "Three Part Aim" as better care, better health, and "lower costs through improvement" while presenting at the National Care Transitions Conference. 
8 By understanding the Triple Aim and its desired outcomes, hospitals can design work processes to meet healthcare quality goals. 7 The purpose of the Triple Aim is to improve healthcare and healthcare delivery in the United States while controlling costs. Berwick intends to implement the IHI's Triple Aim while at the CMS. With Berwick's move from the Institute for Healthcare Improvement (IHI) to the CMS, it could be anticipated that some of the concepts from the IHI would be incorporated into CMS reporting requirements. 5 Donald Berwick recommended extending data transparency to "all aspects of care including science, costs, outcomes, processes and errors." 6 As reporting requirements increase, healthcare organizations will be challenged to collect the most accurate data possible and improve patient care based on those data.Īnticipating changes in reporting requirements may be one way healthcare organizations can be prepared. 4 If quality of care isn't measured, how can success be determined? In the future, successful outcomes will be measured on quality of care and patient outcomes. The Institute of Medicine in 2001 recommended that patients and their families have access to information regarding a hospital's performance on safety, evidence-based practice, and patient satisfaction. 3 Now, performance data from hospitals, home care, and long-term-care facilities are available on the CMS website for patients and families to review. For example, in 2005 the Centers for Medicare and Medicaid Services (CMS) began to publicly report hospital performance data. 2 Quality measurement data are now transparent to the general public, as well as other healthcare organizations, and being used to stimulate healthcare providers to improve quality. Accountability is in the form of decreased reimbursement for low performers in healthcare quality. 1 Mandatory quality reporting and reimbursement incentives have been drivers to encourage hospitals to improve patient outcomes. The October 2010 Regulatory Readiness column discussed how healthcare organizations are challenged to improve care and patient outcomes while decreasing cost. Understanding its components will help healthcare organizations be better prepared to meet the challenges of ever-increasing quality reporting requirements. The Triple Aim is one such driver, with its goal of improving patient outcomes and healthcare delivery. 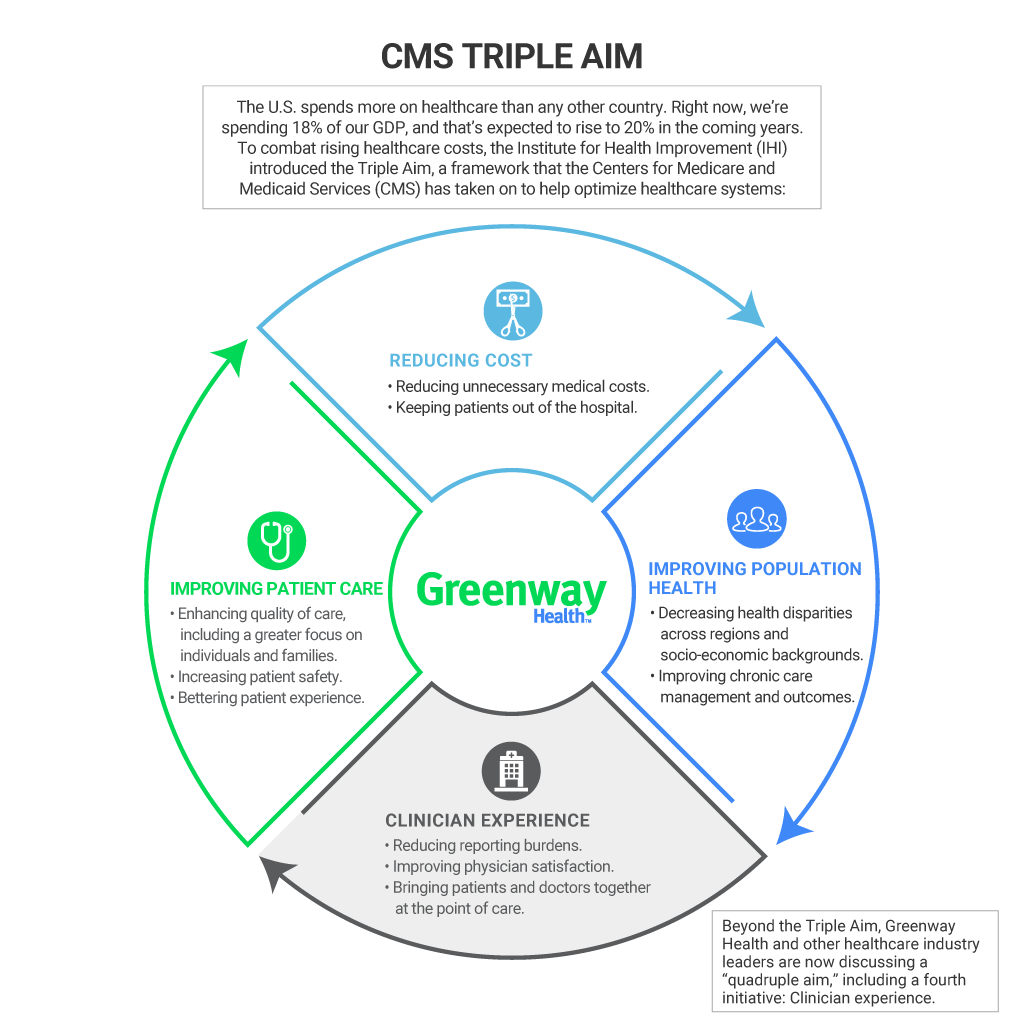
Nurse leaders today are challenged with understanding the drivers behind quality reporting initiatives and meeting reporting requirements.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
